Gout Hates Your Joints
If an illness can have a stereotype, gout has one: its poster boy is a portly, wealthy gentleman who drinks too much red wine and eats too much rich food. In literature, gout is an Epicurean affliction, the runoff of opulence and “disease of kings.”
In fact, gout attacks the poor as well as the rich; it’s more like a creepy shadow that follows other diseases, piggybacks off of their risk factors, and kicks sick people when they’re down. It is also becoming more common.
Studies by Johns Hopkins rheumatologist Allan Gelber, M.D., Ph.D., M.P.H., and internal medicine fellow Stephen Juraschek, M.D., Ph.D., have shed new light on how gout is linked to kidney disease, obesity, cardiovascular disease and high blood pressure. In troubling findings, they also have shown that half of all Americans who take medicine for gout are insufficiently treated. I recently interviewed both of them for a story for Leap, a magazine for the Johns Hopkins Division of Rheumatology.
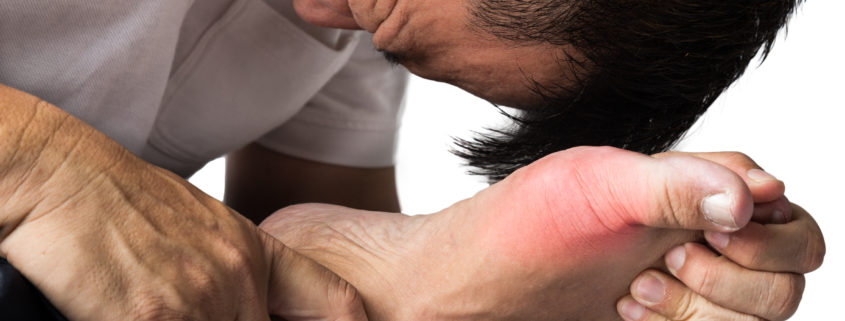
Gout is caused by hyperuricemia, an excess of uric acid (this is a byproduct of the body’s processing of substances called purines). Some foods – yes, including alcoholic beverages and red meat, just as the sterotype suggests – are high in purines, and changing your diet can lower uric acid a little. But for many people, this is not enough. The problem is that uric acid makes crystals, which can build up in the joints. Sometimes this results in a “flare,” an acute experience characterized by redness, tenderness, swelling, and terrible pain. But that’s just the tip of the iceberg, and treatment for the flare is different from treatment for the chronic problem.
Unfortunately, many people – including some doctors – think that treating the acute flare is sufficient. It’s not.
When it’s not screaming for attention, gout moves silently, still forming crystals, and – think of termites – wreaking unseen havoc. “Gout can cause severe damage over time if the uric acid crystals are not cleared,” says Juraschek, “because the crystals can cause degradation and erosion of the bone structure, can cause deformities and lead to super infections over the joint. It is a progressive illness.”
The gout flare itself is incredibly painful, says Gelber. “I’ve heard patients say it was the most incapacitating experience they’ve ever had, more excruciating than a kidney stone or childbirth. The body feels like it’s on fire, because when those crystals come out of the bloodstream and deposit in the joint, it incites an extreme inflammatory response: hot, swollen joints, tophis (which look like small nodules) in the skin. Neutrophils and other inflammatory mediators swarm into the joint, turning it bright, beet red. Fire-engine red. During the worst pain, people might not be able to bear weight on the joint and get out of bed.”
Other diseases such as lupus can produce similar symptoms, and sometimes gout is misdiagnosed. This is where understanding the risk factors comes into play – because gout keeps bad company, and is intrinsically tied to the risk factors of heart disease, including high levels of lipids, high blood pressure, high glucose level, and diabetes.
Gout attacks are fairly common on the medical and surgical services in Johns Hopkins Hospital, says Gelber, who is often called in to see these patients. Typically, someone has a heart attack, comes to the hospital, is treated, free of chest pain and starting to recover, and it’s Day 3. “All of a sudden, that person is in pain, with a hot, red, swollen toe. It’s like gout is kicking people when they’re down.”
After the flare subsides, if the uric acid is not brought under control with long-term medication, gout can go on to cause arthritis that can result in the need for a joint replacement. “Gout is the single most common form of inflammatory arthritis in the U.S.” Although it is more common in men, the risk rises exponentially in women after menopause, he adds.
Gout is on the upswing in America. Juraschek and Gelber, recently explored this issue using data from tens of thousands of Americans in the National Health and Nutrition Examination Surveys. Their research resulted in four papers published in PLoS, co-written with Laura Kovell and Edgar Miller. Here’s some of what they found:
Gout lurks in the risk factors of heart disease and stroke. There is more gout in people who have uncontrolled high blood pressure, and cardiovascular disease risk factors including obesity, high cholesterol, diabetes, and kidney problems. Gelber and Juraschek reported that hyperuricemia was present in 6 to 8 percent of healthy adults, in as many as 15 percent of those with uncontrolled blood pressure (BP), in about a quarter of people with uncontrolled BP plus one extra cardiovascular risk factor (uncontrolled BP plus diabetes, for example), and in as many as 37 percent of those with uncontrolled BP and two additional risk factors. Gout was successively greater, as well, in as many as 12 percent of people with high BP and two risk factors.
Gout goes up with a higher Body Mass Index (BMI) and obesity. The likelihood of gout goes up incrementally with every bit of weight you gain. “The risk with morbid obesity is more than four times higher,” says Gelber, “but it’s one and a half times higher even in people who are just overweight.”
Gout risk rises with impaired kidney function. Close to one-third of people with the highest stages of kidney disease are at risk for gout. “We were surprised,” says Juraschek, “at how high the prevalence is among U.S. adults with kidney disease. That finding really highlighted this overlap in conditions.”
And finally: Half of all Americans who have been diagnosed with gout and who take medicine are not lowering uric acid enough. It’s not clear why: it may be that people don’t take their medicine as directed, or that they stop taking it. The bottom line: “Even though we have good drugs for gout and patients get to the doctor and are treated for it, the medical community achieves suboptimal care,” says Juraschek. “They don’t monitor their treatment.” Which means that if you have been put on medicine to lower your uric acid, you need follow-up bloodwork from time to time to make sure your uric acid level gets to a healthy level and stays there.
Although gout was neglected in medical research for decades, Gelber notes, that has changed. “Since 2000, there has been a tremendous explosion in gout-related research, and in the last 10 years, several new drugs have become available to manage gout, both acutely and chronically. This reflects our improved understanding of the mechanism of gout.”
And yet, says Juraschek, the number of Americans with gout continues to rise, reflecting the rise in obesity and other risk factors. “For doctors, it may not be adequately on the radar – realizing who’s at risk, and taking steps to prevent it.”
©Janet Farrar Worthington


Leave a Reply
Want to join the discussion?Feel free to contribute!